There are likely two reasons behind this controversy:
Gluten Sensitivity
This is often referred to by other names such as Non-coeliac Gluten Sensitivity and Gluten Intolerance. Gluten in the diet is speculated to cause a range of adverse effects, including abdominal pain and bloating, lethargy, lack of concentration, excessive wind and fluctuations from abnormal bowel habits including constipation and diarrhoea. Patients with gluten sensitivity do not have an allergy to gluten in the true pathological sense, but they report an improvement in their symptoms if gluten is removed or reduced in their diet.
It is important to remember that many signs and symptoms of gluten sensitivity are the same as other medical conditions (some which can be quite serious, including gynecological and other gastrointestinal conditions). If you are unwell with any of the above issues, it is imperative to have medical assessment to rule out serious medical conditions and establish the possible cause of your ill health
In Gluten Sensitivity, no allergic or autoimmune reaction is noted. All pathology tests essentially return normal results. It is usually a diagnosis of exclusion, meaning that all known possible diseases have been tested for thoroughly, and excluded. If the symptoms resolve on a gluten-free diet and return upon a gluten challenge, the diagnosis is cemented even further.
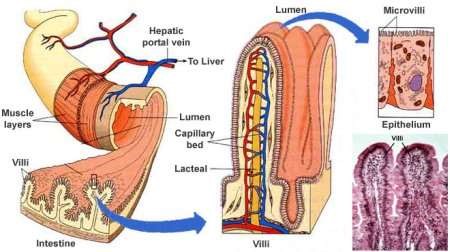
Conversely, Coeliac Disease involves injury to the microstructure of the small intestine, essentially the 'lining' of the small intestine (see diagram below). Microscopic, finger-like projections known as villi and microvilli (responsible for nutrient absorption) are destroyed. Under the microscope, a person with active Coeliac Disease will have no visible villi projecting into the lumen (the hollow space) of the small intestinal tract. Also present will be numerous white blood cells and other immune cells characteristic of inflammatory and allergic response.
Additionally, eliminating gluten-containing foods does remove large food groups from the diet, and appropriate healthy food replacements should be discussed with a health professional to eliminate the possibility of nutritional deficiencies. This is especially important in children, pregnant women and the elderly.
At present, no blood or other pathology tests definitively establish a diagnosis of gluten sensitivity. It is very possible that gluten sensitivity is transient, with certain, even individually unique factors provoking episodes of digestive illness following gluten ingestion.
Factors that may provoke gluten sensitivity and be self-limiting include:
Written by Annalies Corse BMedSc, BHSc.
References
The Gastroenterological Society of Australia (2016). Coeliac Disease. Available at: http://www.gesa.org.au
Dodou, K and Whitely, P (2014). Non-coeliac gluten sensitivity — a look at the evidence behind the headlines. The Pharmaceutical Journal. Available at: http://www.pharmaceutical-journal.com/news-and-analysis/features/non-coeliac-gluten-sensitivity-a-look-at-the-evidence-behind-the-headlines/11132494.article
Ferdu, E (2009). Between Celiac Disease and Irritable Bowel Syndrome: The "No Man's Land" of Gluten Sensitivity. Available at: http://www.nature.com/ajg/journal/v104/n6/abs/ajg2009188a.html
Holmes, G. (2013). Non coeliac gluten sensitivity. Gastroenterology and Hepatology; From Bed to Bench. Available at: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4017515/
Kagnoff, M. (2007). Celiac disease: pathogenesis of a model immunogenetic disease. JCI Insight. Available at: http://www.jci.org/articles/view/30253
 Stay connected and keep up to date with the latest in Functional Medicine
© 2025 | mindd.org | All rights reserved
Stay connected and keep up to date with the latest in Functional Medicine
© 2025 | mindd.org | All rights reserved